What is the No Surprises Act?
The No Surprises Act (NSA) is set to impact medical billing companies due to the significant workflow adjustments required by hospitals and insurance providers. With hospitals facing potential fines of up to $10,000 for non-compliance, revenue cycle management (RCM) service providers must now exercise greater caution in billing and claims processing.
Traditionally, these service providers have managed out-of-network costs through balance billing. However, the NSA will ban balance billing in most states, forcing hospitals, medical billing companies, and insurance providers to swiftly adapt their practices to meet the new legal requirements.
This shift will also bring about changes in the revenue cycle workflow. From determining whether state balance billing laws or the federal NSA applies to a specific case, to calculating shared costs and reimbursement rates, medical billing companies will need to engage with payors and negotiate out-of-network payments with insurance companies.
Addressing the challanges
Real-time Cost Estimation
HealthFAX™ provides accurate, instantaneous good faith estimates, enhancing transparency and patient trust.
Automated Compliance
Built-in compliance checks ensure all billing practices align with NSA regulations, reducing risk and improving accuracy.
Enhanced Communication
HealthFAX™ facilitates clear, timely communication between all stakeholders, reducing confusion and delays in the billing process.
Intelligent Coding and Authorization
AI-driven coding and automated prior authorizations improve accuracy and speed up reimbursement processes.
Features
HealthFAX™ is an Advanced AI-Driven Data Intelligence Platform that addresses the challenges posed by the No Surprises Act and optimizes Revenue Cycle Management.
Real-time Cost Estimation
Generate accurate, instantaneous good faith estimates using AI analysis of vast amounts of medical-financial data. Provide personalized estimates tailored to each patient's specific insurance plan.
Seamless Integration
Effortlessly integrate with existing systems, ensuring smooth data flow between departments. Support for FHIR, HL7, and JSON formats for maximum interoperability.
Automated Compliance
Built-in compliance checks ensure that all billing practices align with No Surprises Act regulations, reducing risk and improving accuracy in billing processes.
Enhanced Communication
Facilitate clear, timely communication between all stakeholders - providers, insurers, and patients. Reduce confusion and delays in the billing process.
Intelligent Coding and Authorization
AI-driven coding and automated prior authorizations improve accuracy and speed up reimbursement processes. Reduce errors and optimize revenue capture.
Clinical Intelligence
Leverage AI to extract valuable insights from unstructured medical notes, streamlining documentation processes and improving decision-making.
Technology

Gen-AI and NLP
HealthFAX™ leverages cutting-edge language models and natural language processing to unlock insights from unstructured medical data, revolutionizing patient care and operational efficiency.
Clinical Intelligence
Transform raw data into actionable clinical insights, empowering healthcare providers with data-driven decision support to enhance diagnostic accuracy and treatment outcomes.
Intelligent Automation
Streamline workflows and eliminate manual errors with smart automations that handle routine tasks, freeing your staff to focus on high-value patient care activities.
API
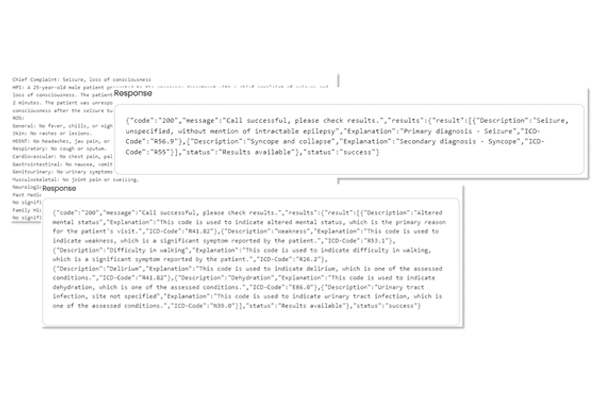
API Interface
Seamlessly integrate our robust functionality with your existing systems to leverage powerful data tools, driving improved operational efficiency and superior outcomes.
- Seamlessly integrate HealthFAX™'s powerful functionality with your existing systems
- Interoperable with support for FHIR, HL7, and JSON formats
- Access to advanced AI technology for healthcare
